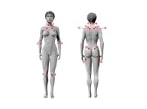
Fibromyalgia, is a mysterious syndrome that is taking an increasing toll on our population. In some instances it is very similar to that of Chronic Fatigue Syndrome. Fibromyalgia is often associated with widespread pain that is often incapacitating and usually affects women in the 25-60 demographic. Fibromyalgia literally means pain in the muscular and connective tissues.
The cause of FMS is unknown and affects over 6 million North Americans. For many years the identification of fibro was very perplexing, because no blood work or other lab tests could show any conclusive evidence. Subsequent studies have shown a common thread of pain patterns and associated symptoms. Pain or point tenderness in the areas of head, neck, shoulders, upper back, elbows, ribs, buttocks, knees and legs is often associated with the syndrome. In addition to pain symptoms there is also sleep pattern disturbance, TMJ syndrome, irritable bowel, chronic headaches, dizziness, sensitivity syndrome, numbness in the extremities, and the list goes on.
With all these symptoms how does one make a diagnosis or evaluation? Usually lab work is negative and actual identification is difficult therefore many victims are anxious and perhaps even depressed because of the lack of concrete evidence. Most patients will have 11 of the 18 points of tenderness and widespread pain in all four quadrants for a duration of three months or more.
Causes of FMS are still very much unknown however there appears to be some common clinical histories. Many patients have been involved in an even a minor motor vehicle accident (untreated), emotional or physical stress, hormone imbalance, nervous system interference, or nutritional component.
Current treatment regimens that include medication and drugs are not all that successful. It is my opinion that a multi-disciplinary approach to the syndrome is key to its management. First off—everyone should be evaluated to establish if they have nerve interference called vertebral subluxation. Chiropractic is exclusive in its mission to detect and remove subluxations. In addition to chiropractic, nutritional balance and support is showing very promising results.
Supplements like MSM assist in managing pain. Exercise geared at stretching muscles and improving cardiovascular is helpful. Relaxation techniques and massage therapy is helpful. Our approach also includes physical therapy, and evaluation of the feet by our foot specialist to ensure a proper foundation to stand on.
This multidisciplinary approach has provided a solution to a very difficult situation. If you know someone who is suffering from FMS call today.
Chiropractic: The "Only Proven Effective Treatment" for Chronic Whiplash!

Study Says 74% of Chronic Whiplash Patients Improved with Chiropractic. A new study published in the Journal of Orthopedic Medicine not only points out the superiority of chiropractic care for chronic whiplash patients, but also examines which chronic whiplash patients respond best to chiropractic care. The authors begin the paper by explaining that:
"Conventional treatment, of patients with whiplash symptoms is disappointing”. A retrospective study by Woodward et al., demonstrated that chiropractic treatment benefited 26 of 28 patients suffering from chronic whiplash syndrome.
The question was not whether chiropractic was beneficial for acute whiplash patients, but to determine "which patients with chronic whiplash will benefit from chiropractic treatment." The authors interviewed "100 consecutive chiropractic referrals for chronic whiplash symptoms," seven of which were "lost to follow up." They were able to divide the remaining 93 patients into three symptom groups:
Group 1: patients with "neck pain radiating in a ‘coat hanger’ distribution, associated with restricted range of neck movement but with no neurological deficit";
Group 2: patients with "neurological symptoms, signs or both in association with neck pain and a restricted range of neck movement";
Group 3: patients who described "severe neck pain but all of whom has a full range of motion and no neurological symptoms or signs distributed over specific myotomes or dermatomes." These patients also "described an unusual complex of symptoms," including "blackouts, visual disturbances, nausea, and vomiting and chest pain, along with a nondermatomal distribution of pain."
The patients underwent an average of 19.3 adjustments over the course of 4.1 months (mean). The patients were then surveyed and their improvement reported as follows:
Group 1
24% – Asymptomatic
24% – Improved by Two Symptom Grades
24% – Improved by One Symptom Grade
28% – No Improvement
Group 2
38% – Asymptomatic
43% – Improved by Two Symptom Grades
13% – Improved by One Symptom Grade
06% – No Improvement
Group 3
0% – Asymptomatic
09% – Improved by Two Symptom Grades
18% – Improved by One Symptom Grade
64% – No Improvement
09% – Got Worse
In their discussion, the authors made these observations:
"Woodward, et al.,2 found improvement in chronic symptoms in 26 of 28 patients (93%) following chiropractic treatment. Our results confirm the efficacy of chiropractic, with 69 of our 93 patients (74%) improving following treatment.
"Our study suggests that such a group of nonresponders does exist, represented by group 3. The defining characteristics of patients in this group were the full range of neck movement in association with neck pain, bizarre symptoms, female sex and ongoing litigation. The mean age of the group at 29.5 (16-43) was lower than that of the other two groups (mean 36.8, range 18-65).
"The results from this study provide further evidence that chiropractic is an effective treatment for chronic whiplash symptoms. However, our identification of a group of patients who fail to respond to such treatment, highlights the need for a careful history and physical examination before commencing treatment."
References
- Khan S, Cook J, Gargan M, Bannister G. A symptomatic classification of whiplash injury and the implications for treatment. Journal of Orthopaedic Medicine 1999;21(1):22-25.
- Woodward MN, Cook JCH, Gargan MF, Bannister GC. Chiropractic treatment of chronic whiplash injuries. Injury 1996;27:643-645.




Leave a Reply